Bus Brings Free Mammograms to Glen Oaks Women

The bus, equipped with a mammogram x-ray machine, was provided by the American-Italian Cancer Foundation. Photo: Iryna Shkurhan
By Iryna Shkurhan | ishkurhan@queensledger.com
A free mammogram screening bus stood on Union Turnpike in Glen Oaks on Friday, May 19 to give women the opportunity to detect breast cancer.
Any woman living in NYC between the ages of 40 and 47, who hasn’t received a mammogram in the past year, was eligible for the service. Uninsured patients were welcome, and those with insurance did not have to pay a copay and had their deductible waived.
“This mammogram event means a lot to the community, and any other groups,” said Shirly Huang from the Coalition of Asian-American IPA, a sponsor of the event. “It doesn’t matter if they are Asian or Latina, cancer doesn’t care what ethnic group you are in.”
Approximately 20 women made an appointment for a screening, and anyone eligible who was walking by was also able to make an appointment on the spot.
Earlier this month, the United States Preventive Services Task Force (USPSTF) unveiled new guidelines that recommend women get their first mammogram at 40, unless they have a family history of breast cancer or other risk factors which would warrant earlier screening.
USPSTF is an independent panel of medical experts who develop recommendations for preventative services based on the evidence and effectiveness of existing programs. Previously they recommended that women in their 40’s make an independent decision on when to start screening based on medical history and recommended they receive one at 50.
Breast cancer is the most common cancer in the U.S, as well as the second leading cause of cancer death for women, according to the National Cancer Institute. The USPSTF predicts that this new change in guidelines could result in 19 percent more lives saved.
Black women are also 40 percent more likely to die from breast cancer than white women, despite being less likely to be diagnosed with it, according to American Cancer Society. Some factors include high rates of genetic mutations, dense breasts and delays in treatment and diagnosis due to systematic inequalities.

Representatives from SHARE and CAIPA were joined by Council Member Linda Lee. Photo: Iryna Shkurhan
“It is systemic,” said Sharon Browne, an outreach coordinator for SHARE, a nonprofit working to support and educate women who have been diagnosed with cancer. She set up a table at the event to distribute literature and answer any questions.
Browne is a two time survivor of an aggressive form of breast cancer. And despite her preventative efforts to annual mammograms, she detected a lump just two months after a mammogram turned up negative.
“I think it’s of the utmost importance to educate,” said Browne, who recalled an older woman who approached her table and didn’t know that cancer can spread from one part of the body to a distant region. She also said that she has met women who only got their first mammogram in their 50s because they were never informed about the appropriate timeline.
“It’s not their fault,” she said. “They just don’t know.”
In her years of experience, she found that the most impactful way to educate women is community events like this, as well as support groups, doctors visits, TV and 24-hour hotlines where any questions can be asked without limits.
Council Member Linda Lee, who represents swaths of eastern Queens, sponsored the event and also took it as an opportunity to get a mammogram herself.
Sponsors of the event said that there are some certain barriers that get in the way of women receiving consistent preventive care. Some women may be embarrassed by the vulnerability of the screening process for cervical and breast cancers. While others may only want care from a doctor who speaks their language and understands their culture.
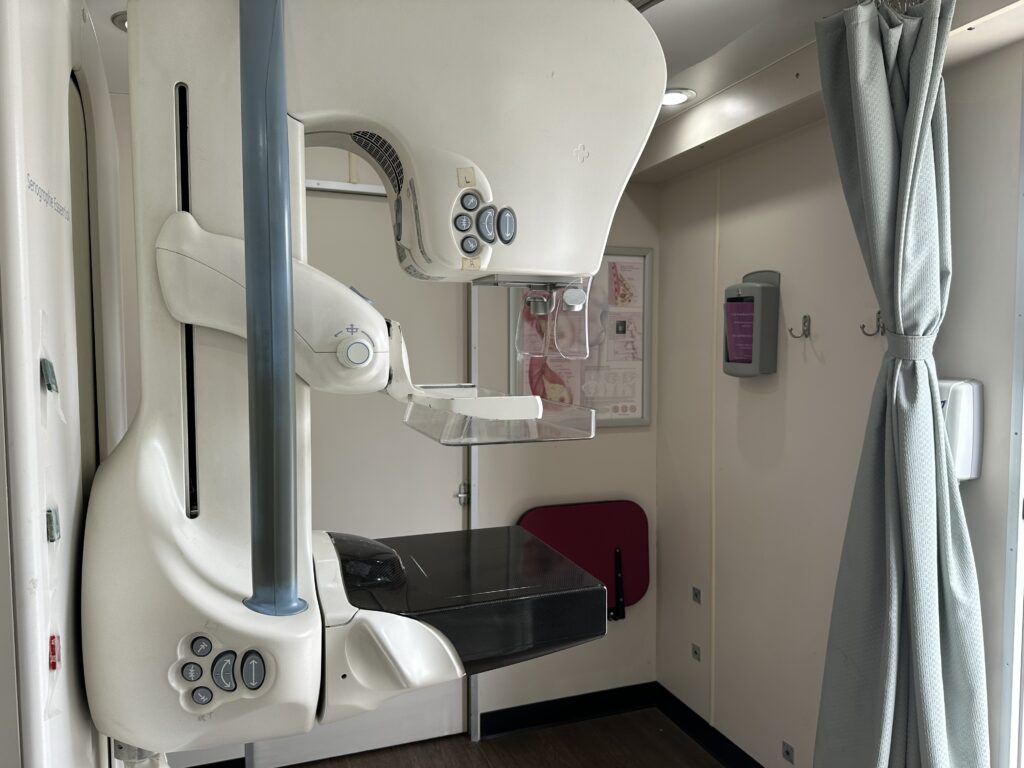
A look inside where the screening takes place. Photo: Iryna Shkurhan
Other women who are more recent immigrants may be uninsured, don’t have the right documents or may have to wait long periods of time for accessible care. Many of the women at the event also acknowledged that life can get busy, which hinders their ability to prioritize preventative care.
The mammogram bus was provided by The American-Italian Cancer Foundation at no cost to patients. Generally, organizers say that it is often booked up and can be found across all five boroughs, five days a week year-round.